Introduction
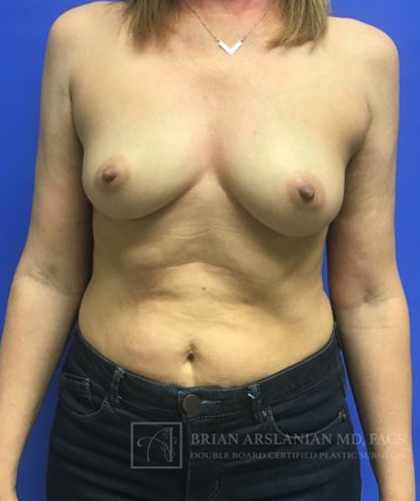
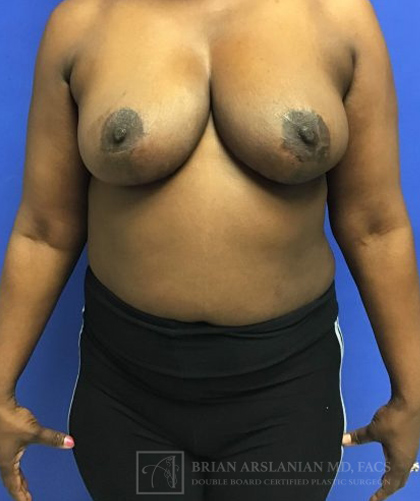
Breast Reconstruction
With 1 in 8 women in the United States developing Breast Cancer, the number of women seeking reconstruction is rising quickly. Whether undergoing a lumpectomy (partial breast removal) or a mastectomy (total breast removal), most women should be given the option to undergo reconstruction. Research continues to show increased psychological benefits for women undergoing breast reconstruction after partial or total mastectomy. Women will often feel better after having such an important part of their self becoming restored. By undergoing reconstruction patients can fill out and feel comfortable in their bathing suits, and will not need to wear a breast prosthesis to fill out their bras.
If you are considering Breast Reconstruction surgery, come and see Dr. Brian Arslanian at Arslanian Plastic Surgery in Atlanta, GA. Dr. Arslanian is a Double Board Certified Plastic Surgeon who specializes in Plastic & Reconstructive Surgery and is ready to work with you. Find out how Dr. Arslanian can help reconstruct your confidence in your body and well-being with a Breast Reconstruction procedure today.